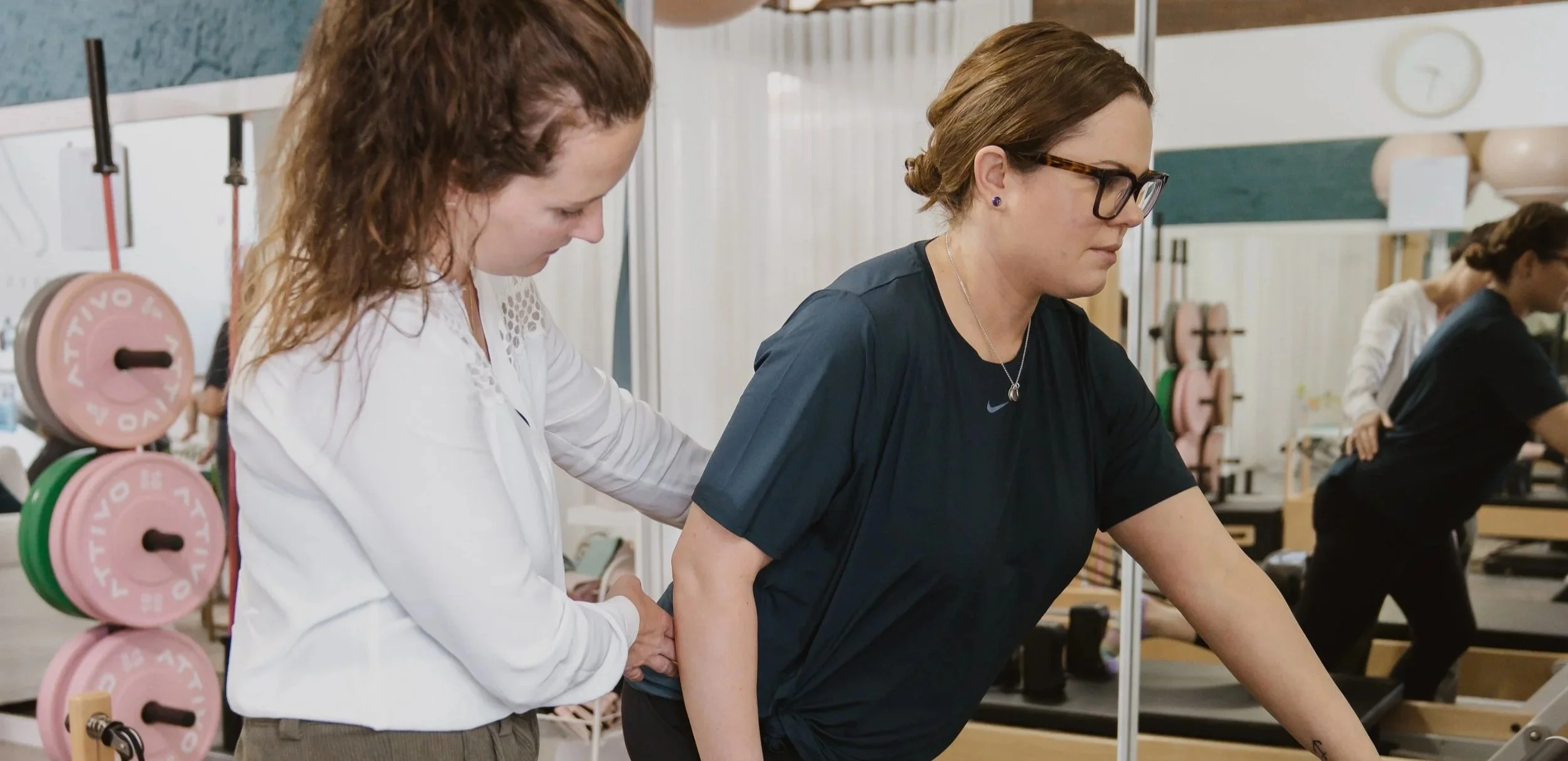
Exercise & Endo (Pelvic Pain)
This article was written for Endometriosis Awareness Month, however many of the concepts discussed apply to persistent pelvic pain more broadly, including pelvic pain affecting people assigned female and male at birth.
Exercise and Endo
Your guide to movement, despite your pelvic pain
Living with pelvic pain, such as Endometriosis, often makes movement feel complicated. Many people notice that exercise helps on some days, yet on other days it seems to trigger fatigue, discomfort, or a full pain flare.
This unpredictability can make it difficult to know which activity or how much activity is helpful, as well as how much might be too much.
At the same time, research shows that exercise is important for managing persistent pain. Hearing that advice while also dealing with symptoms that are exacerbated by certain types or amounts of exercise.
The reality is that exercise can be extremely helpful for many people living with endometriosis and pelvic pain. The key is understanding how pain works and how to approach movement in a way that supports the body rather than pushing against it.
Understand Pain and the Nervous System
To understand why exercise can help, it is useful to understand a little about pain science.
Pain is not something that is directly detected in the body. The body contains specialised nerve fibres that detect information such as pressure, temperature, touch, or chemical irritation. It’s important to know that these nerve fibres aren’t “pain receptors”, they’re detecting information. This process is called nociception. These signals travel to the brain where they are interpreted.
Pain occurs when the brain decides that protection is needed.
This means that pain is not simply a measure of tissue damage. Instead, it is a protective response produced by the nervous system when the brain believes the body may be under threat.
This process takes into account many different sources of information. Signals from tissues are only one part of the picture. The brain also considers context, previous experiences, emotions, stress levels, beliefs about pain, and the surrounding environment before producing the experience of pain.[EG1]
For example, pain can be influenced by factors such as:
Stress and emotional load
Nutrition
Sleep quality
Fatigue
Hormonal fluctuations
Previous injuries or pain experiences
Fear of movement or re injury
The level of physical activity the body is accustomed to
This complexity explains why two people can experience very different levels of pain from the same injury, and why persistent pain can sometimes occur even when tissue healing has already taken place.
Pain and Sensitisation
Conditions such as endometriosis often involve persistent or recurring pain. Over time, the nervous system can become more sensitive to potential threats. This process is sometimes called sensitisation.
When the nervous system becomes more protective, the threshold for triggering pain becomes lower and the intensity of the response can increase.
This does not mean that the pain is imagined or exaggerated. It means that the system has become very effective at protecting the body.
One of the encouraging aspects of modern pain science is that the nervous system is adaptable. Just as it can learn to become protective, it can also learn that certain movements and activities are safe.
Gradual exposure to movement is one of the ways this process can occur.
This graphic shows how pain (the bodies alarm system) can be too protective
@chronicpainproject on Instagram have some really great images to explain this further
Why Exercise Sometimes Triggers Flares
Many people living with endometriosis notice that symptoms can increase after activity. This experience can feel discouraging and may lead people to stop exercising altogether.
In many cases, flares occur when the body is asked to do more than it currently has capacity for.
This can happen when:
Exercise intensity increases too quickly
Activity levels change suddenly after a period of rest
Stress levels are already high
Sleep and recovery have been limited
Hormonal changes increase sensitivity
When the nervous system perceives a potential threat, it may increase protective responses, which can lead to increased pain.
Understanding this helps shift the narrative away from the idea that exercise is harmful. Instead, flares can be viewed as useful information about current capacity.
What Research Says About Exercise and Endometriosis
Emerging research suggests that exercise can play an important role in managing endometriosis related symptoms and improving overall wellbeing.
Studies examining exercise in persistent pain conditions have found that appropriately prescribed physical activity may help to:
Reduce pain severity
Improve physical function
Enhance quality of life
Support mental health
Reduce fatigue
Improve sleep quality
Exercise can influence pain in several ways. Strength training improves muscle capacity and tissue resilience, aerobic activity supports cardiovascular and nervous system health, and movement based rehabilitation helps restore confidence in the body.
For many people living with endometriosis, exercise becomes part of a broader management strategy that supports both physical and nervous system health.
The Best Exercise Is the One You Can Sustain
When discussing exercise for endometriosis, one of the most important factors is adherence.
Research in chronic pain consistently shows that the most effective exercise programs are those that people can maintain over time. Enjoyable and meaningful movement is far more likely to be continued than exercise that feels punishing or overwhelming.
This means that the best exercise is not a single specific method. Instead, the best program is one that feels safe, manageable, and adaptable to the fluctuations that often occur with pelvic pain conditions. This also may mean that the best exercise for one person, will be different for the best exercise for another.
Consistency matters far more than intensity.
Types of Exercise That May Be Helpful
A balanced approach to exercise works best. Our physiotherapists are experts in several different types of movement, and can work with you to establish an exercise program that you will do and enjoy
Progressive resistance training
Strength training helps improve muscle capacity and support around the pelvis, hips, and trunk.
Examples include:
Squats
Lunges
Step ups
Hip bridges or hip thrusts
Rowing movements
Core stability exercises
Strength training improves the body’s tolerance to load and can help people feel more confident in their ability to move.
Low to moderate intensity aerobic exercise
Aerobic activity supports overall health and nervous system regulation.
Examples include:
Walking
Cycling
Swimming
Low impact cardio classes
These activities can improve circulation, support energy levels, and reduce stress.
Pilates based rehabilitation
Pilates based exercise is commonly used in pelvic health physiotherapy because it emphasises controlled movement, breathing, and coordination between the core and pelvic floor.
This approach can help people develop body awareness and movement control.
Mobility and breathing exercises
Gentle mobility work and breathing exercises help reduce muscle tension and support nervous system regulation.
Examples include:
Yoga
Diaphragmatic breathing
Pelvic floor relaxation exercises
Hip mobility drills
Thoracic spine mobility exercises
You can find examples of mobility exercises on our youtube channel here: https://www.youtube.com/@thepelvicstudio/playlists
These types of exercises are often particularly helpful during periods of increased symptoms.
Our small group classes are the perfect environment for supporting exercise with pelvic pain. Find your class here:
Finding the Right Balance
Managing exercise with endometriosis often involves learning how to find a balance between activity and recovery.
Helpful strategies may include:
Starting with small and manageable amounts of movement
Gradually increasing exercise intensity over time
Monitoring symptoms over the following 24 to 48 hours
Incorporating rest and recovery days
Paying attention to sleep, nutrition, and stress levels
This gradual approach helps the nervous system build confidence and reduces the likelihood of large symptom spikes.
Movement Is Empowering
For many people living with endometriosis, movement can become a powerful tool for rebuilding confidence in the body.
Exercise can support strength, mobility, nervous system regulation, and overall wellbeing. It can also help shift the focus from avoiding pain to building capacity.
When exercise is guided and tailored to individual needs, it becomes far more manageable and far more effective.
When Guidance Can Help
Navigating exercise while managing pelvic pain can feel overwhelming. Many people find it helpful to work with a physiotherapist who understands both pain science and pelvic health.
A personalised program can take into account:
Pelvic floor muscle function
Current activity levels
Pain sensitivity
Individual goals and lifestyle
This approach allows movement to be introduced gradually and in a way that feels supportive rather than intimidating.
With the right guidance, exercise can become a valuable part of managing endometriosis and persistent pelvic pain while helping people reconnect with their bodies and the activities they enjoy.
References:
Armour, M., Ee, C. C., Naidoo, D., Ayati, Z., & Chalmers, K. J. (2019). Exercise for dysmenorrhoea and endometriosis-related pain: A systematic review and meta-analysis. Journal of Clinical Medicine, 8(9), 1358. https://doi.org/10.3390/jcm8091358
Geneen, L. J., Moore, R. A., Clarke, C., Martin, D., Colvin, L. A., & Smith, B. H. (2017). Physical activity and exercise for chronic pain in adults: An overview of Cochrane Reviews. Cochrane Database of Systematic Reviews, (4), CD011279. https://doi.org/10.1002/14651858.CD011279.pub3
International Association for the Study of Pain. (2020). IASP revised definition of pain. IASP. https://www.iasp-pain.org
Louw, A., Zimney, K., Puentedura, E. J., & Diener, I. (2016). The efficacy of pain neuroscience education on musculoskeletal pain: A systematic review of the literature. Physiotherapy Theory and Practice, 32(5), 332–355. https://doi.org/10.1080/09593985.2016.1194646
Moseley, G. L. (2007). Reconceptualising pain according to modern pain science. Physical Therapy Reviews, 12(3), 169–178. https://doi.org/10.1179/108331907X223010
Moseley, G. L., & Butler, D. S. (2017). Explain pain supercharged: The clinician’s manual. NOI Group.
Rice, D. A., Nijs, J., Kosek, E., Wideman, T., Hasenbring, M., Koltyn, K., Graven-Nielsen, T., & Polli, A. (2019). Exercise-induced hypoalgesia in pain-free and chronic pain populations: State of the art and future directions. Pain, 160(7), 1441–1449. https://doi.org/10.1097/j.pain.0000000000001381
Slade, S. C., Dionne, C. E., Underwood, M., & Buchbinder, R. (2016). Consensus on exercise reporting template (CERT): Explanation and elaboration statement. British Journal of Sports Medicine, 50(23), 1428–1437. https://doi.org/10.1136/bjsports-2016-096651